Modern Treatments for Varicose Veins that Work
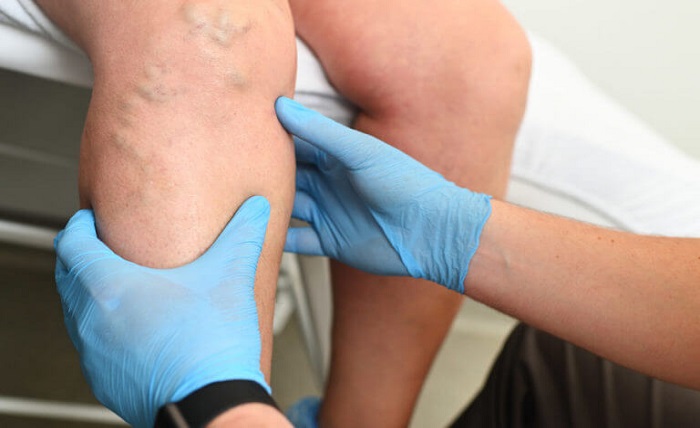
Varicose veins are common yet often misunderstood, appearing as swollen, twisted veins that can cause pain, embarrassment, and, in some cases, serious medical complications. With advances in medical technology, treatment has shifted from traditional open surgery to minimally invasive, office-based procedures that deliver excellent results with significantly less downtime.
This article explains how varicose veins develop, who is most at risk, and which modern treatments are proven to work. It also helps patients understand how to choose the right care path, including when to seek specialized providers such as Metro Vein Centers in North Fort Worth. Written with busy professionals in mind, this guide offers clear, evidence-based insights that can be used confidently before a consultation.
How Varicose Veins Develop and Who’s at Risk
Varicose veins form when one-way valves inside veins fail, allowing blood to pool and stretch the vessel wall. Superficial veins in the legs are most commonly affected because standing and walking increase pressure in those vessels. Contributing factors include age-related wear on valves, genetics, pregnancy (hormonal changes and increased blood volume), prolonged standing or sitting, obesity, and prior deep vein thrombosis.
Who’s at risk? Women are more frequently affected than men, but men still develop symptomatic varicose veins. People with a family history, occupations requiring long periods on their feet, or multiple pregnancies have a higher likelihood. Recognizing risk matters because early intervention, even lifestyle changes and compression, can prevent progression to chronic venous insufficiency, skin changes, or ulcers.
Understanding the mechanism (valve failure and reflux) also clarifies why some treatments target the incompetent segment of a vein rather than every visible bulge. Treating the source of reflux gives longer-lasting results than addressing surface veins alone.
When to Seek Treatment: Symptoms, Risks, and Goals
Symptoms prompting treatment vary. Many seek care for appearance, but common medical complaints include aching, heaviness, leg cramps, swelling, itching, restless legs, and pain that worsens after standing. Left untreated, venous reflux can lead to skin discoloration, lipodermatosclerosis (skin thickening), and venous ulcers, complications that are harder to reverse.
Goals of treatment should be realistic and individualized. They fall into three categories: symptom relief, prevention of progression/complications, and cosmetic improvement. A competent vein specialist will weigh those goals against patient health, anatomy, and lifestyle, aiming for durable relief with the least morbidity. For busy professionals, the best option often balances a high success rate with minimal recovery time so work and travel aren’t disrupted.
Minimally Invasive Procedures with Strong Evidence
Below are the modern, evidence-backed procedures most commonly used to treat refluxing veins.
Endovenous Thermal Ablation (Laser and Radiofrequency)
Endovenous thermal ablation uses heat, delivered by laser (EVLT) or radiofrequency (RFA), to close the incompetent saphenous veins. Under ultrasound guidance and local anesthesia, a thin catheter delivers controlled thermal energy, causing the vein to collapse and scar closed: blood is rerouted through healthy deep veins.
Efficacy: Multiple randomized trials and meta-analyses show closure rates above 85–95% at one year and durable symptom improvement. Recovery is quick: most people return to normal activity within days. Pain and bruising are generally mild. Rare complications include nerve injury or skin burns, but experienced operators minimize these risks.
Mechanochemical Ablation and Cyanoacrylate Glue Closure
These are non-thermal, non-tumescent alternatives. Mechanochemical ablation (MOCA) combines a rotating wire that disrupts the vein lining with simultaneous sclerosant infusion. Cyanoacrylate glue seals the vein mechanically without heat or sclerosant.
Efficacy: Both show closure rates similar to thermal techniques in short- and mid-term studies, with advantages of less post-procedure pain and no need for compression stockings in some protocols. They’re attractive for patients sensitive to heat-related nerve injury or those who prefer to avoid the local tumescent anesthesia used in thermal methods.
Ultrasound-Guided Foam Sclerotherapy
Foam sclerosant (a detergent mixed with gas) is injected under ultrasound into refluxing segments or varicose tributaries. Foam displaces blood and irritates the vessel wall, producing closure.
Efficacy: Foam sclerotherapy is effective for many veins but has slightly lower long-term closure rates for the large saphenous veins compared with ablation. It’s often used for smaller tributaries, residual veins after ablation, or when minimally invasive access is needed. Side effects include temporary pigmentation and, rarely, transient neurologic symptoms.
Ambulatory Phlebectomy for Surface Veins
Ambulatory phlebectomy removes prominent surface varicosities through tiny skin punctures. It’s performed under local anesthesia and often combined with treatment of the underlying refluxing saphenous vein.
Efficacy: Phlebectomy gives immediate cosmetic improvement and durable symptomatic relief for discrete bulging veins. It complements endovenous techniques when surface branches remain after treating reflux.
Comparing Treatment Options: Effectiveness, Recovery, and Costs
Choosing between treatments depends on anatomy, patient goals, comorbidities, and cost considerations.
Factors to Consider When Choosing a Treatment
- Vein anatomy: length and diameter of the refluxing segment and presence of perforator incompetence guide technique selection.
- Symptom severity and cosmetic priorities influence whether single-session phlebectomy is appropriate versus staged ablation plus sclerotherapy.
- Patient factors: pregnancy plans, clotting disorders, peripheral neuropathy, and anticoagulation status.
- Practical concerns: time off work, travel, and tolerance for compression.
Typical Recovery Timelines and Expected Outcomes
- Endovenous ablation and MOCA: return to light activity the same day, normal activity in 1–3 days; exercise progression over 1–2 weeks.
- Foam sclerotherapy: minimal downtime: some aching for a few days; follow-up injections sometimes required.
- Phlebectomy: small wounds with quick recovery: shoes and activity can resume quickly, though bruising may last weeks.
Most modern techniques relieve symptoms and improve appearance significantly; many patients report high satisfaction when the underlying reflux is corrected.
Potential Risks, Side Effects, and How They’re Managed
Common mild effects: bruising, tenderness, temporary numbness, and skin discoloration. Less common but important risks include deep vein thrombosis, phlebitis, nerve injury, and skin ulceration or pigmentation. Prevention uses careful ultrasound mapping, appropriate technique selection, and post-procedure follow-up. When complications occur, early recognition and treatment (anticoagulation for DVT, wound care for skin issues) limit long-term impact.
How to Prepare for a Consultation and What to Ask
A focused consultation saves time and leads to better decisions. Preparation and the right questions ensure the visit is productive.
Key Questions to Ask a Vein Specialist
- What tests will you use to confirm the diagnosis? (A duplex ultrasound is standard.)
- Which vein(s) are causing my symptoms, and which treatment do you recommend and why?
- What are the risks and expected recovery for that option?
- How many similar procedures have you performed, and what are your closure rates?
- Will I need compression afterward or follow-up treatments?
- What are the estimated costs and insurance coverage details?
What to Bring and Diagnostic Tests to Expect
Bring a list of medications, prior vein treatments, and symptom history. Expect a standing physical exam and a duplex ultrasound to map reflux while the patient is standing or semi-erect. A clear plan should follow the imaging results, often with same-day scheduling for office-based procedures if desired.
Choosing a Provider: Credentials, Experience, and Second Opinions
Selecting a provider matters. Look for board-certified specialists in vascular surgery, interventional radiology, or phlebology with focused vein training. Experience with ultrasound-guided procedures and a high case volume correlate with better outcomes. Reviews and before/after photos can be informative, but prioritize measurable outcomes (closure rates, complication rates) and transparent pricing.
Second opinions are reasonable for complex anatomy or if recommended treatments differ from what other credible centers suggest. For professionals who value time, clinics that offer clear pre-visit instructions, online scheduling, and streamlined follow-up are practical. My Profit Engine’s audience, busy entrepreneurs and agencies, might appreciate clinics that provide efficient care coordination and minimal downtime, allowing faster return to work and travel.
Conclusion
Modern treatments for varicose veins emphasize targeted, minimally invasive approaches that correct the root cause, venous reflux, with less pain and downtime than traditional surgery. Endovenous thermal ablation, mechanochemical approaches, cyanoacrylate glue, foam sclerotherapy, and ambulatory phlebectomy each have roles depending on vein anatomy and patient goals. Compression, lifestyle changes, and informed provider selection remain essential parts of good care.
For someone balancing a demanding schedule, the smart path is a focused consultation with ultrasound mapping, a clear discussion of goals, and a plan that minimizes disruption while maximizing durability. With today’s options, most people can expect meaningful symptom relief and improved leg appearance without lengthy recovery, a practical outcome for professionals who need solutions that fit into busy lives.